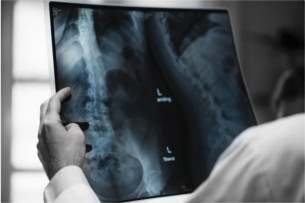
Wrong-Patient Errors Persist
Have you ever wondered, and even gotten slightly annoyed, when you go to the doctor’s office and get asked several times for your name and date of birth? Turns out, there’s a reason for that: This verification process is one way to ensure that you do not get mistaken for another patient.
You’d think that electronic records systems and other forms of health information technology (HIT) would help eliminate this sort of error, but the authors of a paper that was published in the December 2020 edition of Patient Safety investigated and found that “thousands of reports from over 500 healthcare facilities show that HIT-related wrong-patient errors persist.”
“Oops, wrong-patient” is not something you want to hear, especially after a procedure or surgery. Those words should never be uttered. Not by a doctor. Not by a nurse. Not by anyone in the healthcare field. They are so bad that providing any type of medical care or services to the wrong patient is considered a “Never Event.” This means that the event should never happen. The healthcare organization should have safeguards in place to ensure it never happens. And insurance companies (Medicare in particular) will not reimburse healthcare organizations for costs associated with never events. These “oopsies” are just not acceptable on any level.
And yet with the click of the mouse, an error can happen.
While health information technology (HIT) has improved access to health information and made care more efficient, it has also caused “wrong-patient” errors that can lead to “ordering a medication for the wrong patient, documenting in the wrong record, and uploading an x-ray to the wrong record.” Clearly, these sorts of mistakes can have grave consequences.
Types of Wrong-Patient Errors
Prior research in this area identified that the majority of HIT-related errors occur during a clinical procedure.
- Faulty Ordering. Earlier studies point to the ways that “poor usability, fragmented displays, and limited functionalities” contribute to errors in ordering procedures. Efforts have been made to increase the alerts and verifications as well as limit the number of patient charts that a provider has open at the same time. When these errors occur, a patient may end up having the wrong test or procedure.
- Medication administration. Earlier studies recognize the potential for harm that medication errors can have. Researchers have identified flaws in Barcode Medication Administration (BCMA) that can result in significant wrong-patient errors.
Catching Errors in a Timely Fashion
This study, appropriately titled “Health Information Technology-Related Wrong-Patient Errors: Context is Critical” focused on comparing wrong-patient errors that reached the patient with wrong-patient errors that were caught prior to reaching the patient. “This approach affords the opportunity to identify the people, processes, or technology that may effectively enable the identification of wrong-patient errors before reaching the patient. With this knowledge, those specific processes can be shared and may serve to inform performance optimization within healthcare facilities.” They found there were two main ways that errors were identified:
- Often, errors were discovered during conversations between healthcare workers and patients or their family members. “These findings underscore the role of humans as a safety ‘line of defense’ in complex healthcare environments.”
- A pattern emerged as the authors examined over one thousand cases. Regardless of whether the error was connected to radiology, medication, laboratory, or clinical procedure, it was most likely to be discovered during a deliberate review of the information just before or, in some cases, during the clinical activity.
Recommendations
As a result, the authors of the study have the following recommendations.
When it comes to clinical procedures, they suggest:
- Make sure that there are two patient identifiers when ordering medications or procedures.
- Reduce the interruptions that occur during the ordering process and develop strategies for what to do if an interruption is unavoidable.
- Have providers and staff collaborate to determine what “gaps exist” and how they can discover errors before they reach patients.
- Reinforce the importance of reviewing information.
- Consider “specific time-outs or other deliberate pauses”.
When it comes to HIT systems, they suggest:
- Create a work environment that is conducive to being able to focus.
- Develop additional safeguards that can alert clinicians so they can notice the error before it reaches the patient like making facial photographs available to providers.
Clearly, this paper sheds light on some important ways to eliminate wrong-patient errors, or at least ensure that these errors do not reach the patient. If you or someone you love has suffered from a wrong-patient error, call our experienced Cleveland malpractice lawyers to discuss your options for legal recourse and for obtaining the compensation you deserve. To schedule your free consultation, call 216-287-0900 or contact us online today.